The Connection Between
Fascia and Trauma
Your body is making adjustments to best support you and protect you with the resources it has.
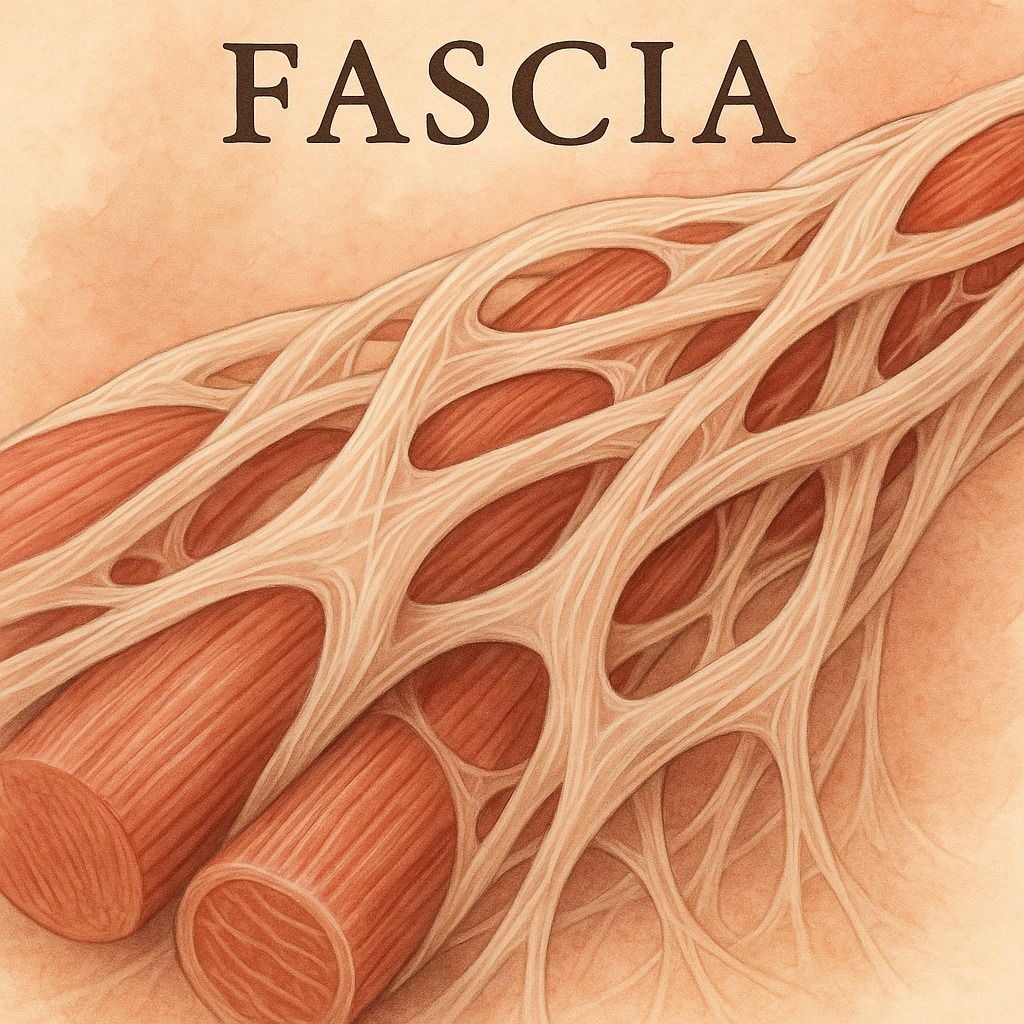
Fascia — the connective tissue that wraps and connects every structure in the body
What If Your Body Is Simply Speaking the Only Language It Knows?
You have discovered breathing exercises, talking therapy, or even medication. These are deeply helpful and essential for your system. And still, your body feels braced — as if something underneath your awareness is protecting you.
What if there is more needed? What if the tension you feel is not a character flaw, but a biological response embedded in the tissue that wraps every muscle, organ, and nerve in your body?
"Fascia is not packing material. It is a sensory organ — richer in nerve endings than skin or muscle."
— Robert Schleip, PhD, Fascia Research Group, Technical University of MunichThis exploration follows the science. No mysticism. No metaphor. Just what peer-reviewed research reveals about how trauma reshapes connective tissue, and how releasing it can change how you feel, breathe, and move through the world.

The body speaks in sensation — fascia is one of its primary voices
Fascia: Your Body's Largest Sensory Organ
Schleip's lab at the Technical University of Munich demonstrated that fascia is richly innervated with mechanoreceptors — especially interoceptive free nerve endings. Fascia houses over 250 million nerve endings, making it one of the most information-dense tissues in the body.
🔬 What Is Interoception?
Sensing the internal state of the body. The more interoceptive input, the more data the brain receives about "How safe am I right now?"
Schleip, R. (2012). Fascia as a Sensory Organ. In Fascia: The Tensional Network of the Human Body.
⚡ Trauma and Interoception
Van der Kolk's research consistently shows altered interoceptive awareness in people with PTSD and anxiety disorders. Their internal sensing becomes either blunted or hypersensitive. The body becomes noisy — or numb.
van der Kolk, B. (2014). The Body Keeps the Score.
Fascia: 250 million nerve endings — the body's largest sensory network
When Stress Rewrites Your Tissue Architecture
Chronic stress increases sympathetic nervous system tone. Elevated cortisol and catecholamines influence fibroblasts — the cells that maintain fascia — increasing collagen cross-linking and tissue stiffness.
🧬 Fibroblast Response
Peer-reviewed findings link psychological stress to changes in connective tissue remodelling and inflammatory markers. Long-term stress literally changes tissue architecture.
⚙️ Myofibroblasts
Fascia contains myofibroblasts — contractile cells. Under sustained tension or inflammatory signalling, they generate tension autonomously. Tension becomes semi-independent of voluntary muscle contraction.
That is not poetic language. That is histology.
Translation: your body can hold tension patterns from past stress — not because you are choosing to, but because the tissue itself has remodelled around that state.

Chronic stress is not just psychological — it rewrites the architecture of your tissue
Your Brain Predicts Danger From Your Tissue
Neuroimaging studies show that trauma alters activity in the amygdala (threat detection), medial prefrontal cortex (regulation), and insula (interoception). The body is interpreted as unsafe.
If fascia becomes chronically tense, interoceptive signalling shifts. The insula receives continuous "compression / threat" signals. The brain then predicts danger.
🧠 Lisa Feldman Barrett's Constructionist Model
Emotions are not reactions — they are brain predictions built from interoceptive input plus past experience. Change the body input, you shift the prediction landscape.
— Barrett, L.F. (2017). How Emotions Are Made: The Secret Life of the Brain.
The loop: Trauma → altered autonomic tone → fascial tension remodelling → altered interoception → altered emotional prediction → anxiety behaviour patterns.
The brain reads the body's fascia signals to predict safety or danger
Breath, Vagal Tone, and the Fascial Highway
Fascia forms continuous lines — including thoracolumbar fascia connecting pelvis, diaphragm, ribs, and neck. When fascial tension increases in the trunk, diaphragmatic excursion decreases.
Restricted Breath
Studies show people with anxiety demonstrate more apical (chest) breathing and reduced heart rate variability (HRV). When the diaphragm cannot descend freely, the breath stays shallow — and the nervous system stays on alert.
Vagal Tone (HRV)
HRV is a measure of vagal tone. Higher HRV correlates with better emotional regulation. Stephen Porges' polyvagal theory connects vagal function with social engagement and safety perception.
— Porges, S.W. (2011). The Polyvagal Theory.

Deep diaphragmatic breathing restores fascial freedom and activates the vagus nerve
What Fascial Release Actually Does
Manual therapy and myofascial release have been shown in peer-reviewed trials to produce measurable shifts in the nervous system.
✦ Evidence-Based Outcomes
- 🔽Reduced sympathetic nervous system activity
- 📈Increased parasympathetic markers, including HRV
- 😌Lower state anxiety scores
- 🧪Decreased salivary cortisol levels
- 💆Improved perceived stress and mood
Randomized controlled trials in fibromyalgia, chronic pain, and anxiety populations. (NIH PubMed)
The mechanism: Pressure on fascial tissues stimulates Ruffini endings — slow-adapting mechanoreceptors linked with parasympathetic activation. Slow, sustained pressure downregulates sympathetic tone.
Slow pressure → vagal engagement → altered breath rhythm → altered brain oscillations → updated emotional prediction.

Slow, sustained pressure on fascia activates parasympathetic receptors and shifts the nervous system
From Brain Waves to Behaviour
Research from Richard Davidson's lab shows that emotional states correlate with specific cortical activation patterns. Anxiety often shows excessive high-frequency beta activity. When autonomic tone shifts toward parasympathetic dominance, alpha activity increases and hypervigilant beta patterns decrease.
🔄 Breaking the Loop
Judson Brewer's work on anxiety demonstrates that anxiety loops are reinforced by interoceptive discomfort plus cognitive rumination. If body tension reduces and breath deepens, the loop loses fuel. The prediction error signal changes. The brain updates.
— Brewer, J.A. (2021). Unwinding Anxiety.
🧍 Posture Is Biology
Studies show upright posture increases positive affect and reduces stress compared to slumped posture. Fascia determines posture more than isolated muscles do. Ida Rolf approached this structurally: align the body in gravity, reduce strain patterns, free breath.
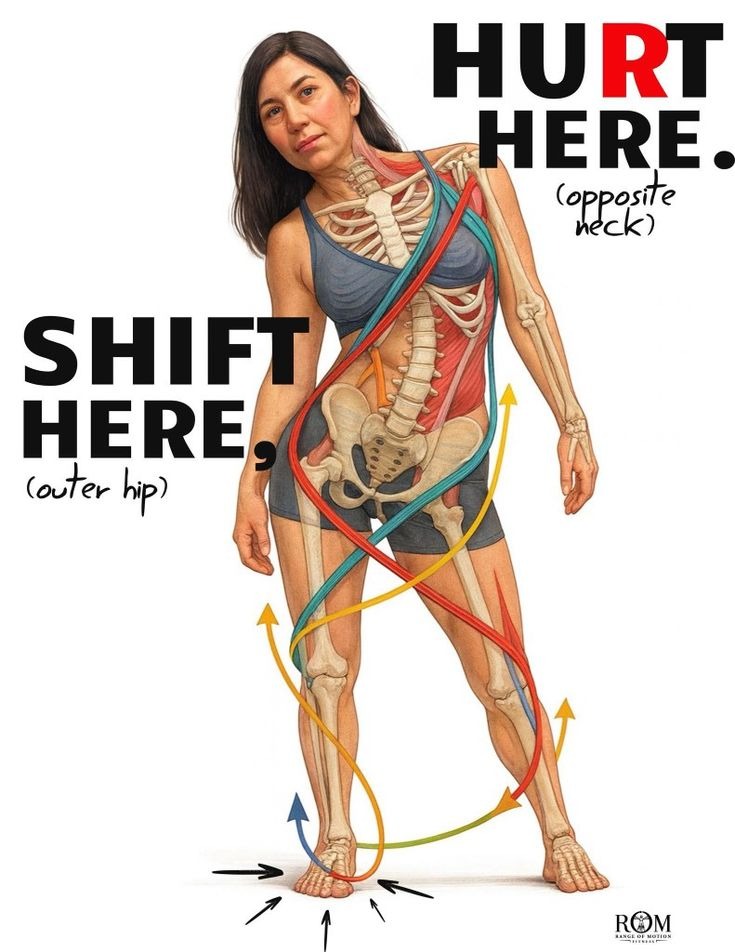
Fascial alignment shapes how you move through the world — and how the world reads you
The Cutting-Edge: Emerging Fascial Science
As Helene Langevin's research (Harvard/NIH) shows, the fascial system is not just "wrapping"—it is a communication network that responds to touch, movement, and held tension.
🪱 Hyaluronan Phase Transitions
Research by Dr. Carla Stecco explores how Hyaluronic Acid (HA) — the fluid lubricant between fascial layers — thickens into a sticky, honey-like substance (densification) due to stress or lack of movement. Newest studies suggest that breathwork, vibration, and localized heat change the pH of the tissue, catalyzing the HA to return to a fluid state.
⚡ Piezoelectricity
Collagen exhibits piezoelectric properties, generating electrical charges when mechanically deformed. Cutting-edge research explores the theory that the fascial web acts as a whole-body, fiber-optic communication system, transmitting bioelectrical signals instantly across the body.
Source: International Journal of Molecular Sciences - Fascia & Hyaluronan

Emerging research reveals fascia as a bioelectric communication network — transmitting signals across the whole body
The Full System
This is not mystical energy. It is mechanotransduction — mechanical input converted into neural and biochemical signalling.
The Pattern
- 1.Fascia is sensory and contractile
- 2.Stress changes tissue tension
- 3.Tissue tension alters interoceptive signalling
- 4.Interoception shapes emotional construction
- 5.Emotional state influences behaviour and social presence
What People Report After Release
- 🫁Deeper spontaneous breathing
- 💧Increased emotional recall or release
- 🌡️Reduced pain sensitivity
- ☀️Improved mood and sense of calm
Van der Kolk documented that body-based therapies reduce PTSD symptoms through restoring bottom-up regulation.
Fascial fibroblasts respond to mechanical stretch by releasing cytokines and growth factors. Mechanical touch influencing inflammatory cascades. Chronic inflammation is strongly correlated with anxiety and depression in meta-analyses.

Clients consistently report deeper spontaneous breathing and improved calm after fascial release
The Honest Frontier
The data is still emerging. Many studies are small sample sizes. Mechanisms are proposed but not fully mapped. That is intellectual honesty.
Working theory, grounded in current evidence: Fascial release may influence anxiety and trauma symptoms by altering interoceptive input, autonomic tone, inflammatory signalling, and breath mechanics — which collectively update emotional predictions and behavioural patterns.
The frontier question now is dosage and specificity. Which techniques? What pressure? What frequency? Which populations respond most? That is where the next decade of research will go.
Everything Is Connected
Fascia is a continuous sheet of connective tissue that runs through the entire body — connecting muscle, bone, nerve, and organ into one integrated system. When load patterns change in the tissue, the nervous system responds. When the nervous system shifts out of a protective state, the tissue can begin to soften and reorganise. This is why physical release and nervous system regulation work together — they are part of the same system.
This is the work of the fascia release therapist — we are both doing the work. It is a collaborative process of listening to the patterns and reorganizing the system together, thread by thread, until ease is restored.
Your body is holding a story.
Let it
finish.
If your body feels braced, alert, or stuck — this is worth paying attention to. It is a fascial pattern worth exploring. Professional fascia release work can begin to interrupt the loop.
🔗 Recommended Exploration
Deepen your understanding of the body-system connection with our specialized series.
View: Blood Sugar Series →066 559 6780
hanlie@hanlietheron.com
hanlietheron.com
Somerset West · Kuilsriver